Introduction
The private health sector, in its diverse forms at all system levels, has increasingly become a key source of essential health services in communities worldwide. As privately delivered services become a more foundational component of national health service offerings, ensuring the quality of that care is now a greater priority for the global community. Quality of care “is a key component of the right to health, and the route to equity and dignity” for women, children, and other health care users.1 Many questions remain around the roles and actions of governments and private entities in assuring and improving the quality of privately delivered health services.
The Sustaining Health Outcomes through the Private Sector (SHOPS) Plus project works closely with governments and private sector partners in diverse global contexts to pursue stronger quality assurance and improvement methods. This brief summarizes the project’s implementation experience to contribute to global knowledge around tested and replicable strategies.
SHOPS Plus shares a range of approaches and experiences in quality assurance and improvement from its work in Madagascar, Nigeria, Senegal, and Tanzania. It provides lessons learned and practical tips for donors who want to support future efforts.
A definition
According to the World Health Organization (WHO), quality of care can be defined as “the extent to which health care services provided to individuals and patient populations improve desired health outcomes. To achieve this, health care must be safe, effective, timely, efficient, equitable and people-centered.”1 To achieve universal health coverage, it is essential to ensure the sustained delivery of health services that meet these criteria.
Any framework for quality of care (in the private sector or otherwise) emphasizes that quality health care is viewed from the level of the provider, at health facilities, at numerous systems levels, and among patients and communities themselves. There are a plethora of interventions that can influence quality of care at any level. The Lancet Commission on High Quality Health Systems in the Sustainable Global Development Era defines a quality health system as “one that optimizes health care in a given context by consistently delivering care that improves or maintains health outcomes, by being valued and trusted by all people, and by responding to changing population needs”.2
Achieving quality of care at the health service delivery level requires, as foundational steps, establishing standards of care, ensuring the continuous availability of essential infrastructure and commodity supply, mobilizing an adequate and skilled workforce, matching appropriate incentives for quality of care to provider motivations, strengthening community involvement in building demand, and monitoring data.3
Quality of care is created through strategic choices in health systems, at health facilities, and among providers and their patients. It requires a focus on assuring and improving the components of safe, appropriately delivered, and effective health products and services.
Challenges and needs unique to the private health sector
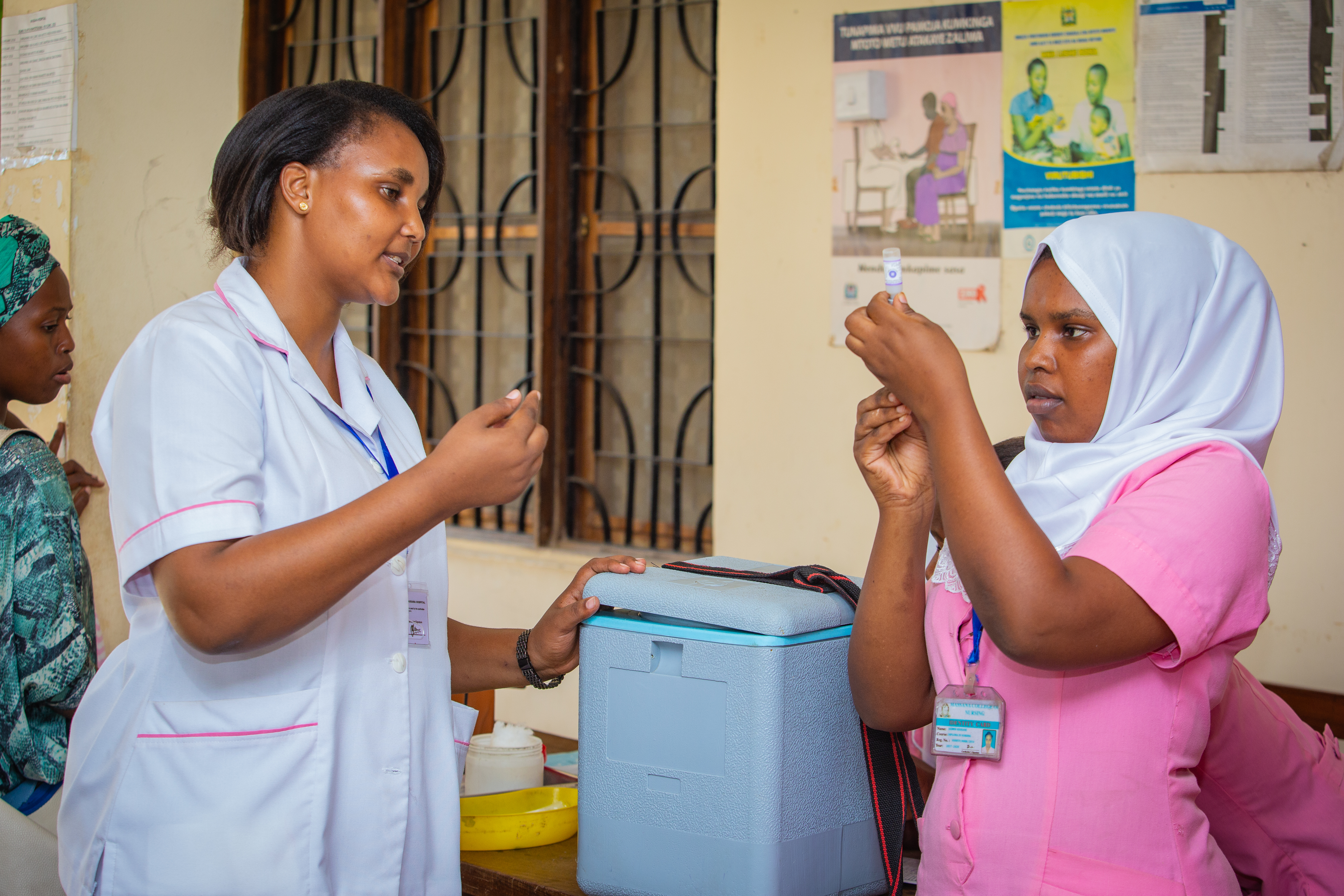
Assuring and improving the quality of health services is a critical priority in the public and private health sectors. Both sectors face similar challenges ensuring that health provider skills and competencies are adequate. Both also lack consistent availability of essential infrastructure, commodities, and other inputs to clinical care. However, the private health sector has unique challenges in addressing gaps in quality. Most countries lack a consistent mechanism for improving the performance of private sector providers. The public sector often has limited capacity to refresh the skills of providers from either sector and provide sufficient oversight.
Various SHOPS Plus private sector assessments have highlighted challenges that private providers experience. The private health sector is often very large and fragmented. Private facilities are often unknown to government regulatory bodies because of poorly enforced licensure and registration regimes, infrequently updated registries, and weakly enforced requirements regarding private facilities’ reporting to public authorities. As a result, private providers are often excluded from government policies, processes, and planning that focus on quality of care. This prevents them from accessing continuing medical education opportunities and government- or donor-led trainings. Private facilities do not receive routine feedback from the public sector or other external oversight bodies on the quality of their services through supportive supervision or other engagement. Finally, because their clients may keep returning, many private providers assume they deliver quality services and lack the incentive to invest in quality improvement activities.
Addressing these challenges to strengthen the quality of health service delivery—in the public or private sector—is best understood as a continuous, multidimensional process. The global literature confirms that comprehensive programs that use several targeted interventions at once are preferred over isolated interventions.3, 4
In Nigeria, SHOPS Plus employs a combination of approaches to improve quality in its family planning program, including a two-week in-service training and post-training engagement. The program was successful due to the incorporation of adult learning techniques, post-training follow-up, and ongoing supportive supervision that built relationships between the providers and local government.
Organizing the private sector
In many countries, private health facilities (for-profit and nonprofit) and their providers operate independently and are often isolated from each other and the national health system. In the absence of formal organization or aggregation, it is an immense practical challenge to effectively engage each private provider or entity independently to assess and strengthen the quality of care for health services. Finding and engaging private providers for quality of care interventions and support requires an organized private health sector. External implementing partners and private providers have sought to address this challenge by creating aggregating bodies (provider or facility associations, formal and informal networks, and social franchises) that reach numerous individual providers and facilities at once to address quality issues. SHOPS Plus refers to private providers and facilities working with these aggregating bodies as networked. Networked private providers and facilities typically benefit from increased accountability, access to health commodities, clinical training, and supportive supervision. Facilities or providers who are non-networked or weakly networked do not benefit from these quality of care inputs except through independent action. Locating these providers in many settings is an immense challenge.
As a requirement for formal health professions in most countries, private health providers of various cadres are aggregated under a professional council or national health profession licensure body. Although such registration bodies demonstrate vastly different authorities and capacities in both assessing and assuring the quality of services, they can be a powerful way for private health providers and facility leadership to organize themselves. The associations serve many purposes. They are representative bodies for advocacy efforts with the government and the public, they disseminate quality of care standards, convene providers for quality assurance and improvement dialogue, and may support the implementation of quality assurance and improvement programs that benefit members. The Integrated Midwives Association of the Philippines successfully advocated for midwives to be accredited with PhilHealth, the national health insurance program.5 Accreditation is an important quality assurance mechanism that ensures providers meet minimum quality standards. PhilHealth covers over 90 percent of the population and not being a PhilHealth-accredited provider is seen as a disadvantage.6 The association operates its own private midwifery schools and offers continuing professional development courses to its members, showing how associations can support quality improvement with knowledge improvement efforts.5
Social franchising has also been a powerful approach to promote care seeking and quality of care among private health providers in numerous global settings. In most cases, social franchising involves organizing private health facilities into a network linked under a common brand. The facilities benefit from a perceived standard of quality associated with that brand. Franchisees benefit from franchisor support such as training, access to commodities, and oversight, while clients feel assured that they are receiving services from a reputable brand. Quality assurance begins in the recruitment stage, as franchisors confirm certification and licensure before inviting a facility into the network. To stay within the network, franchisees must adhere to the standards and systems set in place by the franchisors. Most systems include participation in clinical trainings, adherence to reporting requirements, and participation in regular oversight visits from quality assurance coordinators. Most important, standards are enforced. If a franchisee is not adhering to the quality of care standards and processes, they may be removed from the network. Social franchises also help equip providers to deliver quality services by providing them with commodities and financing to purchase equipment and other resources. Many social franchises help franchisees become empaneled in national health insurance schemes, which often have their own quality standards that facilities are expected to maintain.7

Photo: Javier Acebal
Although private providers and facilities can be aggregated under councils, professional associations, social franchises, or other networks, there is evidence that a large number of private providers and facilities are not working with aggregating bodies or are only weakly connected. The definition of non-networked private providers and facilities varies by country. However, it broadly refers to a private health entity that is formally licensed as a health provider or certified as a registered health facility but is operating independently without any working relationship with the formal health system or other providers in a meaningful sense, and without the supervision, accountability, and quality mechanisms that aggregating approaches can provide. A SHOPS Plus literature review shows that there have been very few interventions specifically targeting these non-networked private providers and facilities, revealing a gap in the global evidence that this brief seeks to address.